TTEC VeriCycle
Turn revenue cycle complexity
into faster, more predictable
cash flow.
TTEC VeriCycle
Turn revenue cycle complexity
into faster, more predictable
cash flow.
Healthcare organizations, Payers and Providers alike, must reduce administrative burden by accelerating claims processing and reimbursements. TTEC VeriCycle automates workflows, prevents unnecessary denials, improves first-pass rates and overall member satisfaction.
Backed by more than two decades of healthcare expertise, we leverage intelligent automation, shift upstream and equip Providers with the interoperability to Payer Systems to provide real-time insights before claims are submitted to the clearing house to address potential issues.
TTEC VeriCycle ACCELERATOR FOR PROVIDERS
Our solution supports the full revenue cycle, from patient access to payment reconciliation.
Verify eligibility, check benefits, and automate prior authorizations to reduce manual work and prevent billing errors.
AI-assisted coding extracts clinical data, validates payer rules, and improves claim accuracy before submission.
Automated claim validation and submission ensure cleaner claims and faster payer processing.
Analytics identify denial patterns while AI generates appeal letters to increase recovery rates.
TTEC VeriCycle ACCELERATOR
FOR PROVIDERS
At the point of Claim Entry
- Reduction in claims rework and repeat contacts by 5 to 10% year 1 and continued significant improvement in subsequent years
- First-contact claim resolution with 95%+ accuracy
- NPS Improvement in overall member and/or provider experience
- Eligibility issues, PA issues, denial reasons caught up front – reduction by 5 to 15% Year 1 and continued significant improvement in subsequent years
- Denial prevention from a provider standpoint as opposed to denial management
- Low Interoperability costs vs high integration costs.
- TTEC VeriCycle Intervention points
- Patient Registration
- Insurance Verification
- Pre-Authorization
- Clinical Documentation
- Claim Creation and Submission
- Clearing House Validation
- Claim Adjudication
- Payment Posting
- Denial Management and Appeals
- Reporting & Performance
Pre-service Acceleration
Intake & Registration
Scheduling / referrals, patient registration, demographics validation
Coverage Verification
Eligibility + benefits verification, COB checks
Authorization & Medical Necessity
Prior auth initiation/tracking, medical necessity validation
Patient Financial Readiness
Estimates, financial counseling/coverage discovery, pre-service collections
Coding & Charge Integrity
Documentation & Charge Capture
Documentation completeness, charge capture, reconciliation
Coding Production
ICD-10/CPT/HCPCS coding (facility + professional)
Coding Quality & Compliance
QA, audits, compliance validation
Revenue Integrity Controls
Edits, leakage detection, exception routing
Cash & Denials Optimization
Claims Management
Claim creation, edits/scrubbing, submission, rejections/resubmission, status follow-up
Denials & Appeals
Denials prevention, denials management, appeals drafting/submission/tracking
Payments & Reconciliation
ERA/EOB ingestion, posting, exceptions, reconciliation, credit balances/refunds
A/R & Collections
A/R segmentation, work queues, follow-up, patient billing support, collections/bad debt
TTEC VeriCycle in the contact center
Member and provider inquiries flow through the agent + VeriCycle, which calls payer systems APIs
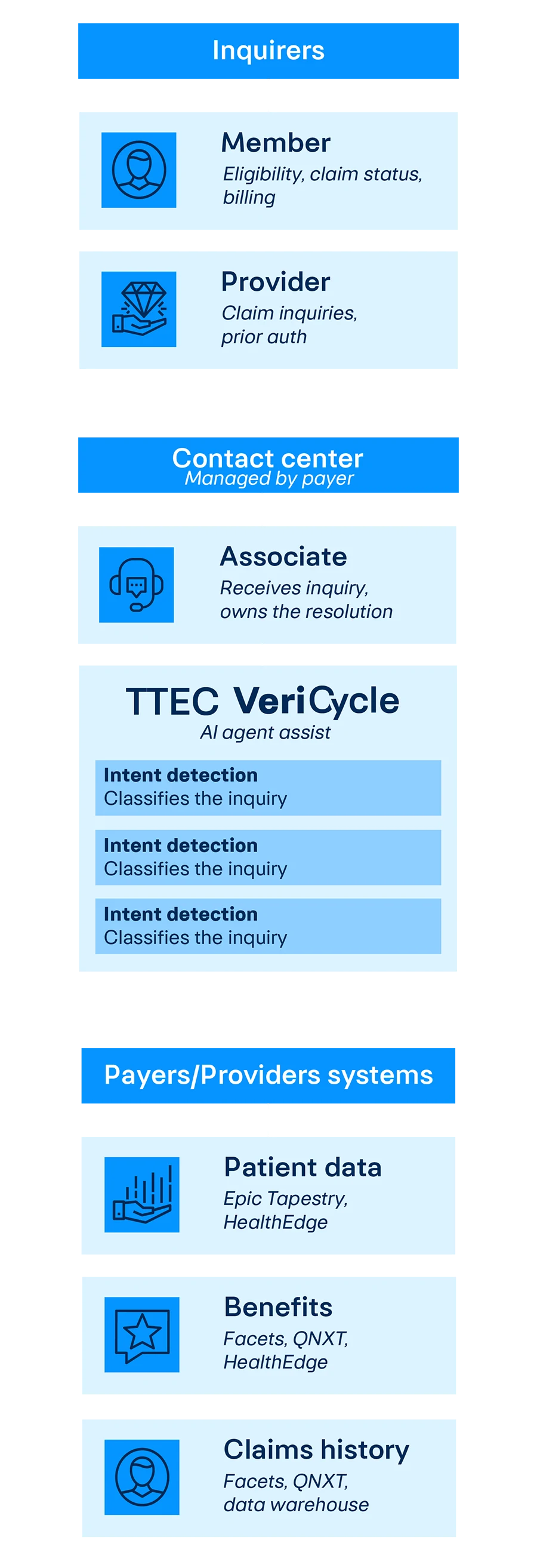
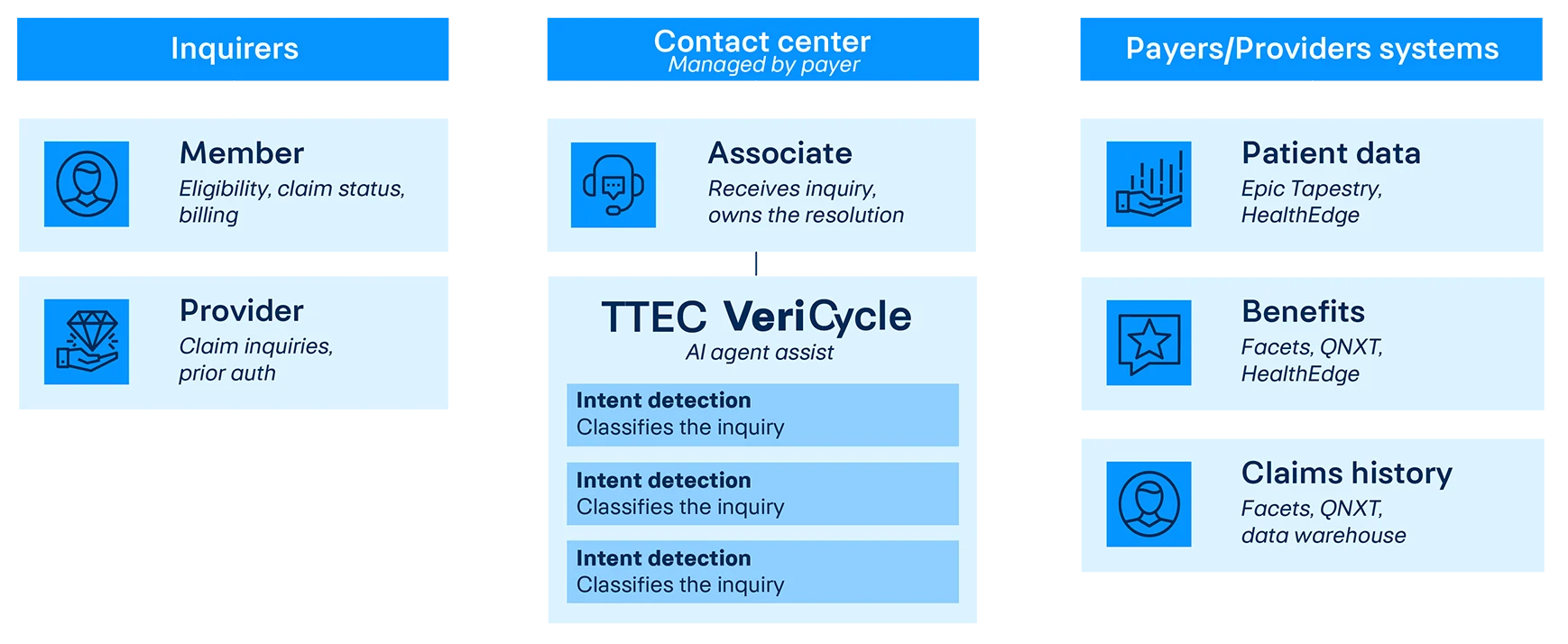
From inbound contact
to resolution
—Six steps, all happening in parallel with the live conversation

Step 1
Inbound Contact
We support retail banking, wealth management, digital transformation, fraud, and lending operations to improve experience and efficiency.

Step 2
Agent + VeriCycle launch
TTEC VeriCycle opens alongside the agent's desktop, attached to the conversation in real time.

Step 3
Intent detection
Classifies the inquiry: eligibility, claim status, prior authorization, or appeal.

Step 4
Knowledge retrieval
Calls payer APIs in parallel — FHIR R4 for patient data, X12 270/271 for eligibility, X12 276/277 for claim status.

Step 5
Next-best-action
Consolidates results, surfaces the relevant policy and history, and recommends the resolution path.

Step 6
First-call resolution
Agent closes the inquiry on first contact with accurate, current data — driving down AHT, lifting FCR.
Why TTEC?
Why
TTEC?
Real-time revenue
insights
Accelerate reimbursement
Reduce manual
work
Gain full visibility
Prevent denials before
they happen
Deploy quickly
26+ Healthcare clients
7.1K+ Healthcare advocates globally
Built for accuracy. Designed for speed.
Fewer errors. Faster answers. Better outcomes.