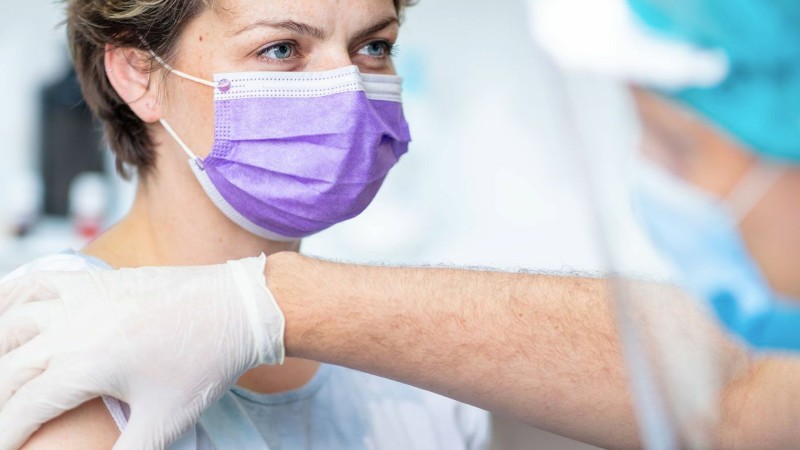
In part 1 of our series on the role customer experience plays in accelerating COVID-19 vaccine efforts, Ann Marie Muñana, a nursing and healthcare leader at Chamberlain University and member of the Chicago Department of Public Health’s Scientific COVID-19 Vaccine Work Group, shares strategies for earning the trust of vaccine skeptics, ideas for maximizing vaccine resources, and other insights.
Key Takeaways:
- More work is needed to combat misinformation about the COVID-19 vaccines
- Community-level intervention and word-of-mouth communications are effective tools but there needs to be a cohesive approach
- Nursing students are an underutilized resource for administering the vaccine and assisting in other areas
Judith Aquino: Hi, welcome to the CX Pod. I'm Judith Aquino. Today we'll be discussing the customer experience factor as it relates to the COVID-19 vaccines and efforts to increase the vaccination rate. Joining me in this discussion is Ann Marie Muñana, a nursing and healthcare leader at Chamberlain University. Ann also serves on the Chicago Department of Public Health Scientific COVID-19 Vaccine Work Group. Welcome to the show, Ann.
Ann Marie Muñana: Thank you. Thank you very much. I'm so pleased to be here today.
JA: Let's start by talking a little bit about the Vaccine Work Group. Can you tell me what is its purpose and has it accomplished so far?
AM: Sure, absolutely. The work group was put together by our leaders at the Chicago Department of Public Health, our healthcare commissioner, Dr. Allison Arwady. And it includes a number of area experts, physicians, scientists, nurses, ethicist statisticians who look at the data that was coming to the FDA, to the Food and Drug Administration as their process to do the emergency authorizations for the first two vaccines, the Pfizer vaccine and the Moderna vaccine.
And so our goal was to you know, make sure that we were comfortable with how the process was going because there's been so much dialogue and so much focus on the speed at which the vaccine was developed, that it was important to have members of the Chicago healthcare community support the vaccine in order to improve and increase the distribution, or actually the vaccine acceptance rate that is so important. We can have a vaccination, but if people are not getting the vaccine, you know, that's a problem. So we were lending our expertise and our voice to the Department of Health to confirm that we feel that the FDA did what the FDA needs to do in order to issue the emergency authorization.
JA: And have you seen any results yet, from your efforts?
AM: Well, our findings, our summary, our results are published on the Chicago Department of Public Health’s website and basically just confirming and holding and supporting the findings from the FDA and the safety of the vaccine. And so our hope is to now, as we move forward, to reach out and be a part of the community effort to encourage and to educate our community on the importance of the vaccine and its safety.
JA: And what are you finding is key to engaging the community and also combating the misinformation that's out there?
AM: One of the challenges that we've seen is just the huge amount of information from all areas, right? It's from the television, from the internet, from family members, from friends. There's just so much information that it is daunting for some of our patients and members of our community to sort through and to understand. And so our responsibility and our duty as healthcare providers, as clinicians, as doctors, nurses, and other members of the team, is to be the voice of our patients and to help them understand and help them make that decision that they need to make in order to accept the vaccine and take the vaccine. And so I think one of the challenges has been all that information. I think there's been a disconnect in perhaps some of the leadership on do this, don't do this and, and people changing their opinions. So it is very confusing and that's going to be one of the challenges that we face is to make sure that we are messaging correctly. And appropriately.
JA: Are there any lessons that have been learned from distributing other vaccines that might help such as the flu, hepatitis B, or HPV vaccines?
AM: I think the lessons that are learned every step of this process is important. Every element from the vaccine development to the trials and the men and women who volunteered for the trials. And then now onto the distribution, it's all very, very important. And I must say we certainly have been impacted by some things as straightforward as the temperature of the vaccine and how that has impacted the distribution. And so I think it's important that not only do we commit the resources to our scientists and our labs and our you know, pharmaceutical company labs to develop the vaccines, but we also have to be very, very on top of the distribution and what that means. And when we say we're going to have, you know, a million vaccines, well, that's also a million bandaids, a million needles, a million alcohol swabs, and that whole process needs to come together. I think communication is another lesson that we need to make sure that we're being responsible in our communication and being accurate. And if we don't know the answer, then we don't know the answer. And we find out the answer.
JA: I’d like to go back to in terms of engaging the community and addressing the concerns of different groups as the vaccine is rolled out. So there've been reports that even healthcare workers are refusing the vaccine. What would you say is really important to, to appeal to that type of patient?
AM: You know, I'm so glad that you asked that question. It's hugely important. I mean, at this point it's about taking the vaccine and accepting the vaccine, and we realize that there are some of our members of the community, some people that they will never take the vaccine for whatever reason. And I think what our challenge is is that larger sector of the population that's in the gray area that they have hesitancy. And so when we, when we ask the individuals in our community, you know, what is it that gives you pause? What makes you hesitant? Many of them, it's not so much that they're not going to take it, but many of them want to wait and see, well, I want to see how it goes. And I want to get more information about it.
I want to understand the long-term effects about it. I want to make sure that it's safe. And, and so for that part of the population, I think it's more of a wait and see kind of approach that we're taking in terms of us addressing that as a nurse. And we are such a trusted profession. And as a nurse, we have a responsibility to educate our patients as role models. And for us to also get the vaccine, I am troubled by healthcare workers who have chosen at this time not to be vaccinated. And I think we'll have to really go a little deeper and try to find out why that is, what their reasoning is. However, I am very encouraged as time goes by that as people, you know, let me step back a second. When you tell someone, you know, 20% of people had this and 50%, when we give them numbers, it's hard for someone to really put their arms around that and just sort that out. And so what seems to be making a difference is a personal connection. So when you say, you know what, my neighbor got the vaccine and she is fine, or my teacher or my doctor, or my nurse, that in a way, makes a larger impact on the individual when they feel like they've known someone who got the vaccine and did okay. So I think as we get the vaccine rolled out as more and more people take the vaccine that hopefully we will see that word of mouth, if you will.
JA: Are there any misconceptions that you encounter in terms of where we are with getting the vaccine?
AM: I think there are probably misconceptions. One of the things perhaps is even the way with the speed that the development has gone. Yes, it has been a speedy development of a vaccine. Absolutely. However, that was part of what our work group was looking at is to, do that, to put our eyes on the data and on the information and give reassurance that just because something went quickly, that there weren't any corners cut. I mean, our scientists were, and researchers were, you know, 24/7 around the clock, just like our healthcare providers in the hospital for the last 10 or 11 months. I've been taking care of patients 24 hours a day, seven days a week. So the effort was put into it and the work was done appropriately. However, you know, there are individuals that will just, you know, they have their mind made up and they have their opinions and I respect their opinions. But, but perhaps we can still do better about messaging and about providing reassurance.
JA: And looking ahead, do you see this becoming part of a playbook that could potentially be used? Heaven forbid we have to face another pandemic like this, but I'm just wondering what would be the key takeaways from this experience?
AM: Well, you're absolutely right. I mean, I know we're talking about lessons learned and God forbid we ever have to deal with this in our lifetime again, but I do think that we need to find a way to have a more cohesive approach whether it's you know, I love our country and the individuality of our states and how we were founded. Each state has their own, you know, governor, and then we have our federal government, but I think there's an opportunity there to see if we can map out improved communication and improved cooperation so that it does get down to that individual, to that city, to that county, to that city, to that community.
JA: Great. And my last question for you is, so our new president said he wants to administer a hundred million doses of the coronavirus vaccine in his first hundred days in office. What, and I know you alluded to this a little bit earlier, but what would be your advice to him to make that happen?
AM: I, you know, I support that. I think that is a manageable goal. I think it's going to take a lot of work and I would say, you know tap into all the resources that are needed. And you know, as someone who is a nurse educator, you know, we can throughout the United States, the multiple, the many nursing students who are there, who are able to help in this effort, our medical students, our pharmacy students are, you know, there's, there's a lot of people who are here that want this to succeed. And so I know with nursing programs, we're working very closely with our national nursing organizations to make sure that our nursing students are counted among those who can participate in the vaccination efforts.
JA: Ann, thank you so much for sharing your insights with me. I really appreciate it.
AM: Thank you very much. It was my pleasure.